What is Male Infertility?
Male infertility occurs when a man’s body struggles to produce healthy sperm or deliver sperm to a woman’s egg. Think of sperm as tiny swimmers: if they’re too few, move sluggishly, or have odd shapes, pregnancy becomes difficult. Surprisingly, 40% of infertility cases in couples involve male factors, and over 60–80 million couples worldwide face infertility challenges. Despite its prevalence, many people don’t understand what causes it or how to address it.
Key Fact: Sperm health isn’t just about quantity—it’s about quality. Even men with normal sperm counts can face infertility if their sperm can’t swim properly or have damaged DNA.
How Common is Male Infertility?
About 1 in 10 men experience infertility. However, cultural stigma often keeps this issue hidden. For example:
- In some regions, infertility is blamed solely on women, leaving men untreated.
- Many men avoid medical help due to embarrassment or lack of awareness.
Did You Know?
- Up to 50% of cases have no clear cause (called “idiopathic infertility”).
- Lifestyle factors like smoking, obesity, and stress worsen sperm health over time.

Book a Free Consultation Today – Your Journey Starts Here!
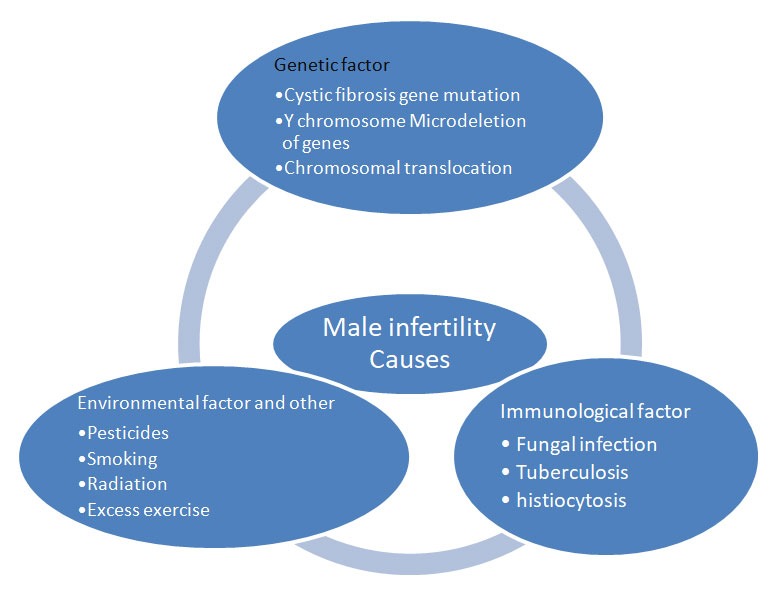
Causes of Male Infertility
Let’s break down common causes in simple terms:
- Hormonal Imbalances
Hormones like testosterone, FSH (follicle-stimulating hormone), and LH (luteinizing hormone) control sperm production. Imbalances can occur due to:
- Pituitary gland disorders (e.g., tumors).
- Thyroid problems (overactive or underactive thyroid).
- Steroid abuse (common in athletes).
- Genetic Issues

Some men inherit conditions that affect fertility:
- Klinefelter Syndrome: Extra X chromosome (XXY) leads to small testicles and low testosterone.
- Cystic Fibrosis: Causes missing vas deferens (tubes that carry sperm).
- Y Chromosome Deletions: Parts of the Y chromosome, crucial for sperm production, are missing.
- Blockages (Obstructive Causes)
Sperm might be healthy but stuck due to:
- Infections: STDs like chlamydia can scar reproductive tubes.
- Injury: Trauma from accidents or surgeries (e.g., hernia repair).
- Birth Defects: Missing vas deferens or epididymis (sperm storage ducts).
- Lifestyle and Environmental Factors
- Smoking: Damages sperm DNA and reduces motility.
- Alcohol: Heavy drinking lowers testosterone.
- Obesity: Fat cells convert testosterone to estrogen, harming sperm production.
- Heat Exposure: Hot tubs, tight underwear, or laptops on laps raise scrotal temperature.
- Toxins: Pesticides, lead, and radiation harm sperm.
- Medical Conditions
- Diabetes: High blood sugar damages blood vessels and nerves in the reproductive system.
- Varicocele: Swollen veins in the scrotum (like varicose veins) overheat the testicles.
- Cancer Treatments: Chemotherapy and radiation often destroy sperm-producing cells.
Symptoms of Male Infertility
Most men feel perfectly healthy, but red flags include:
- Testicular Pain or Swelling: Could signal infection or varicocele.
- Low Semen Volume: Less than ½ teaspoon (1.4 ml) per ejaculation.
- Ejaculation Issues: Pain, delayed ejaculation, or retrograde ejaculation (sperm enters the bladder).
- Small or Hard Testicles: May indicate hormonal or genetic problems.
Important: Many men discover infertility only after failed attempts to conceive. Regular check-ups are crucial!
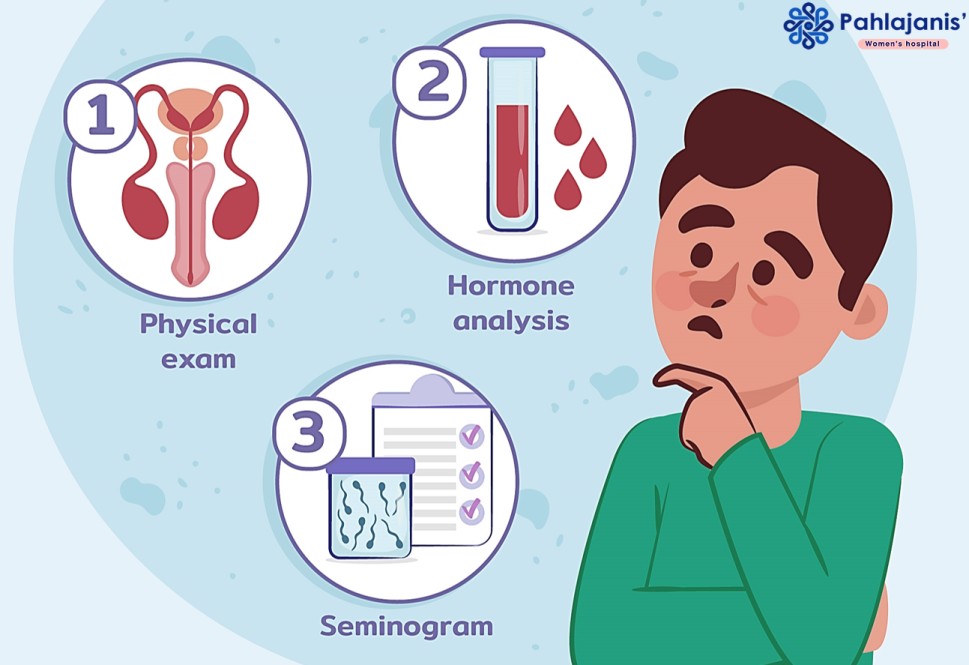
Tests for Male Infertility
Doctors use these tests to diagnose issues:
- Semen Analysis: Normal Semen Parameters (As per WHO 2025 Criteria)
| Semen Parameter | Lower Reference Limit |
| Sperm Volume | 1.4 ml |
| Sperm Concentration | 16 million/ml |
| Total Sperm Count | 39 million/ml |
| Total Motility (PR+NP%) | 42% |
| Progressive Motility (PR) | 30% |
| Sperm Morphology | 4% |
- Hormone Blood Tests
- Testosterone: Low levels suggest hormonal issues.
- FSH and LH: High FSH may mean testicles aren’t responding to hormones.
- Physical Exam
- Check for varicoceles, blockages, or testicle abnormalities.
- Ultrasound
- Scans the scrotum for blockages or swollen veins.
- Genetic Testing
- Identifies Y chromosome deletions or cystic fibrosis genes.
Azoospermia: When There’s Zero Sperm
Azoospermia affects 1% of men and has two types:
- Obstructive Azoospermia (OA)
- What Happens? Sperm is produced but blocked from exiting.
- Causes: Infections, vasectomy, or congenital blockages.
- Treatment: Microsurgery to unblock tubes or retrieve sperm for IVF.

- Non-Obstructive Azoospermia (NOA)
- What Happens? Testicles produce little or no sperm.
- Causes: Genetic disorders, hormonal imbalances, or cancer treatments.
- Treatment: Hormone therapy or sperm extraction (TESE, PESA) combined with IVF/ICSI.

Treatments for Male Infertility
- Lifestyle Changes
- Quit Smoking: Improves sperm count in 3–6 months.
- Healthy Diet: Zinc (nuts, seafood), folate (leafy greens), and antioxidants (berries) boost sperm health.
- Exercise: Reduces obesity and stress. Avoid cycling >5 hours/week (harms sperm).
- Medications
- Clomiphene: Boosts testosterone and sperm production.
- Antibiotics: Treat infections like prostatitis.
- Bromocriptine: Lowers high prolactin (a hormone that reduces testosterone).
- Surgery
- Varicocele Repair: Fixes swollen veins, improving sperm count in 60–70% of cases.
- Vasectomy Reversal: Reconnects sperm tubes (40–90% success depending on time since vasectomy).
- Sperm Retrieval: TESE (testicular biopsy) or PESA (needle aspiration) for IVF/ICSI.
- Assisted Reproductive Technology (ART)
- IUI (Intrauterine Insemination): Washed sperm is placed directly into the uterus.
- IVF (In Vitro Fertilization): Eggs and sperm are combined in a lab; embryos are implanted.
- ICSI (Intracytoplasmic Sperm Injection): A single sperm is injected into an egg—ideal for severe cases.
Emotional Impact and Support
Infertility can cause stress, depression, and relationship strain. Ways to cope:
- Counseling: Therapists specializing in fertility can help couples communicate.
- Support Groups: Organizations like RESOLVE (US) or Fertility Network UK offer community support.
- Open Conversations: Normalize discussions about male infertility to reduce shame.
Prevention Tips
- Avoid Toxins: Wear protective gear around chemicals.
- Stay Cool: Skip hot tubs and tight underwear.
- Manage Stress: Yoga, meditation, or hobbies can lower stress hormones.
- Regular Check-Ups: Early detection of issues like varicoceles improves outcomes.

Breaking the Stigma
In many cultures, infertility is seen as a “woman’s problem,” but men are equally responsible. To change this:
- Educate Communities: Schools and media should teach that infertility is a medical issue.
- Celebrity Advocacy: Stars like Chrissy Teigen and John Legend openly discussing IVF help normalize the conversation.
- Policy Changes: Governments should fund fertility treatments and research.
FAQs About Male Infertility
Que. Can vaping cause infertility?
Ans. Yes! E-cigarettes reduce sperm motility and damage DNA.
Que. Does age affect male fertility?
Ans. Sperm quality declines after 40, but men can father children later than women.
Que. Can weight loss improve sperm health?
Ans. Absolutely! Losing 5–10% body weight boosts testosterone and sperm count.
Pahljanis’: Your Partner in Building Families
Pahljanis’ IVF Centre in Raipur is a trusted name in fertility care, offering hope to couples struggling with infertility. Known for its advanced technology and compassionate approach, the center provides personalized treatments like IVF, ICSI, and fertility assessments. With a team of skilled doctors and a focus on affordable, ethical care, Pahljanis’ helps couples navigate their journey to parenthood. Whether addressing male infertility, recurrent pregnancy loss, or complex cases, the center combines cutting-edge science with emotional support, making it Raipur’s go-to destination for modern reproductive solutions.
Visit our website or clinic to start your family-building story: https://pahlajanis.com/best-ivf-center-in-raipur/
Male infertility is a complex but treatable issue. With advancements in IVF, ICSI, and microsurgery, millions of couples now have hope. By understanding causes, seeking early testing, and embracing lifestyle changes, men can take charge of their fertility. Let’s erase the stigma—infertility is a medical condition, not a personal failure. Together, we can build a world where every couple has the support they need to grow their family.